Our research is focused on female-specific conditions that are related to cardiovascular disease (CVD) risk. Currently, we have two main lines of inquiry.
The role of menopause and physical activity on CVD risk
Cardiovascular disease (CVD) risk increases to a greater degree during the transition to menopause than at other times in a woman’s life. Blood pressure, obesity, and cholesterol have all been shown to increase in midlife women from the pre- to the postmenopausal years. The increase in CVD risk factors leads to greater risk of CVD-related events such as heart attack and stroke. Interestingly, there is a growing awareness that conventional CVD risk factors such as blood pressure and cholesterol may underestimate a woman’s risk for cardiovascular disease. Therefore, our lab is interested in evaluating non-traditional risk factors for CVD such as blood vessel health in midlife women.
The focus of our studies is to evaluate the cells that line the inner layer of the blood vessel, called endothelial cells. Endothelial cells are essential to blood vessel health because they are responsible for 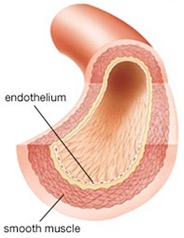 dilating blood vessels when blood flow increases and keeping cholesterol from sticking to and getting into the blood vessel wall. In fact, damage to endothelial cells is the first event in the process of atherosclerosis, which leads to CVD. It has been shown that postmenopausal women have lower endothelial function compared with premenopausal women, independent of aging. We were interested in evaluating the role fitness may have on endothelial health in women at different menopausal stages.
dilating blood vessels when blood flow increases and keeping cholesterol from sticking to and getting into the blood vessel wall. In fact, damage to endothelial cells is the first event in the process of atherosclerosis, which leads to CVD. It has been shown that postmenopausal women have lower endothelial function compared with premenopausal women, independent of aging. We were interested in evaluating the role fitness may have on endothelial health in women at different menopausal stages.
In addition to changes in traditional CVD risk factors such as increased cholesterol, blood pressure, and obesity, menopause is also associated with hot flashes. Hot flashes are experienced in about 70% of women around the menopause transition. The incidence and severity of hot flashes may be associated with early risk of CVD. We are investigating whether habitual physical activity and high cardiorespiratory fitness influences this relationship.
If you are interested in finding out more about this study, contact us here.
The influence of race and ethnicity on blood vessel function
Arterial stiffness is an indicator of vascular health and a strong predictor of future cardiovascular events and all-cause mortality. There are large ethnic and racial disparities in cardiovascular disease (CVD) risk. For example, non-Latino Black women have a higher burden of CVD risk factors than other gender and racial/ethnic groups. Underlying causes of these disparities are unclear but may include health behaviors, access to care, and stress from everyday lived experiences.
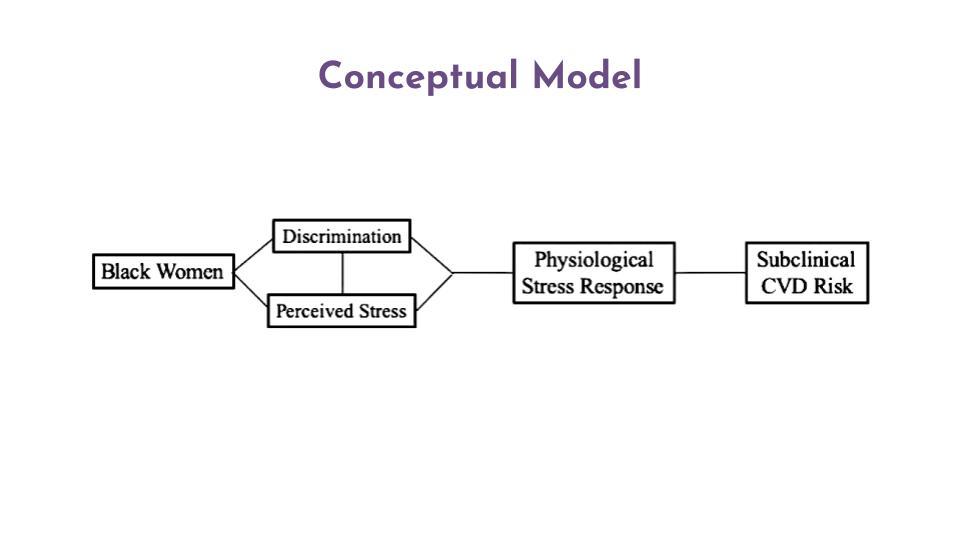
We measure arterial stiffness in the lab through evaluating the wave pulses of blood through the vessels. One bout of physical exercise is known to reduce blood pressure, improve affect, and reduce stress. A single bout of exercise may be one way to reduce arterial stiffness, but it is unclear
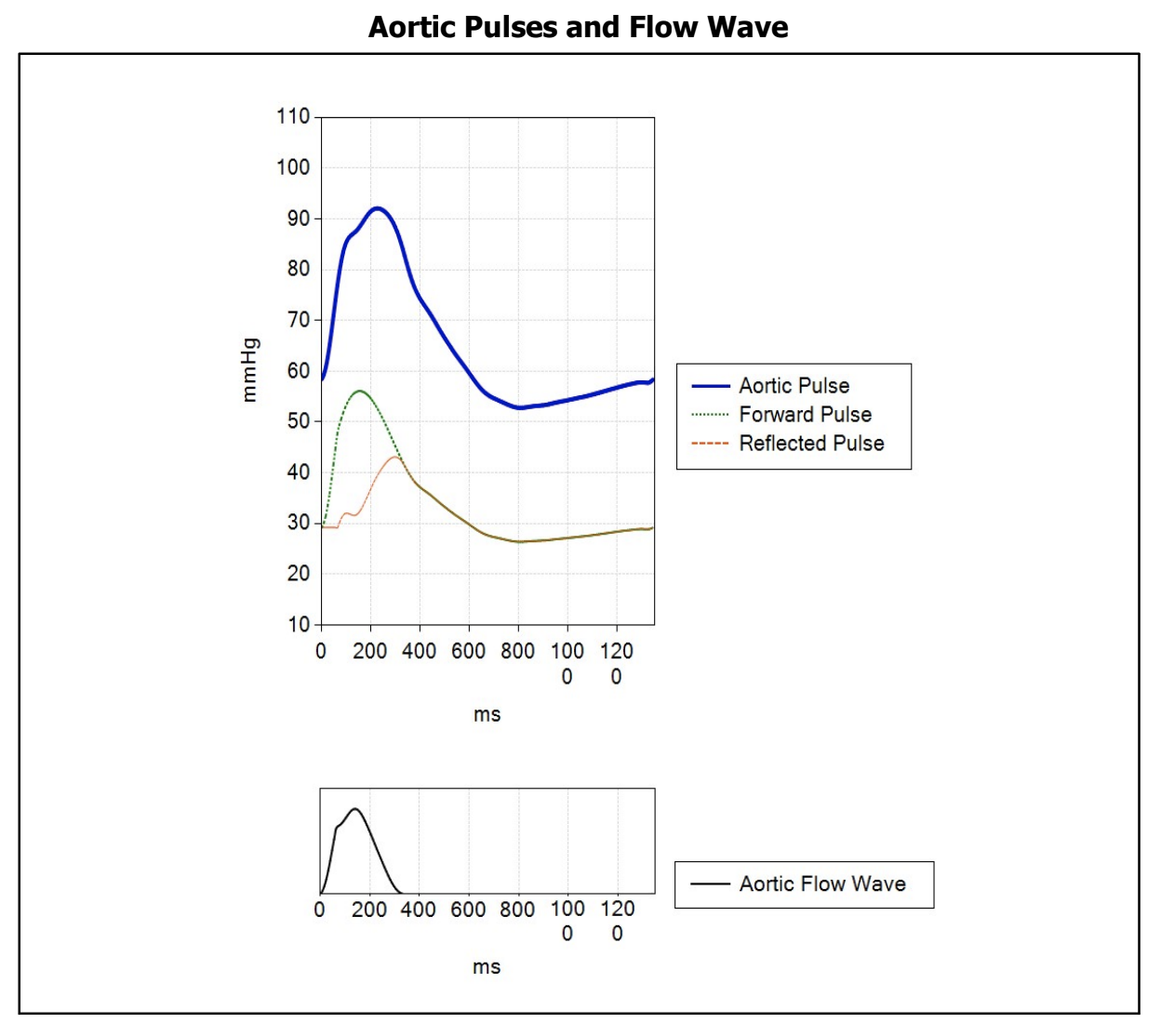
whether this response occurs similarly in women of different racial and ethnic groups. Our work focuses on evaluating the differences in arterial stiffness in healthy women of differing racial and ethnic groups and the effect of one bout of exercise on arterial stiffness.
If you are interested in finding out more about this study, contact us here.
